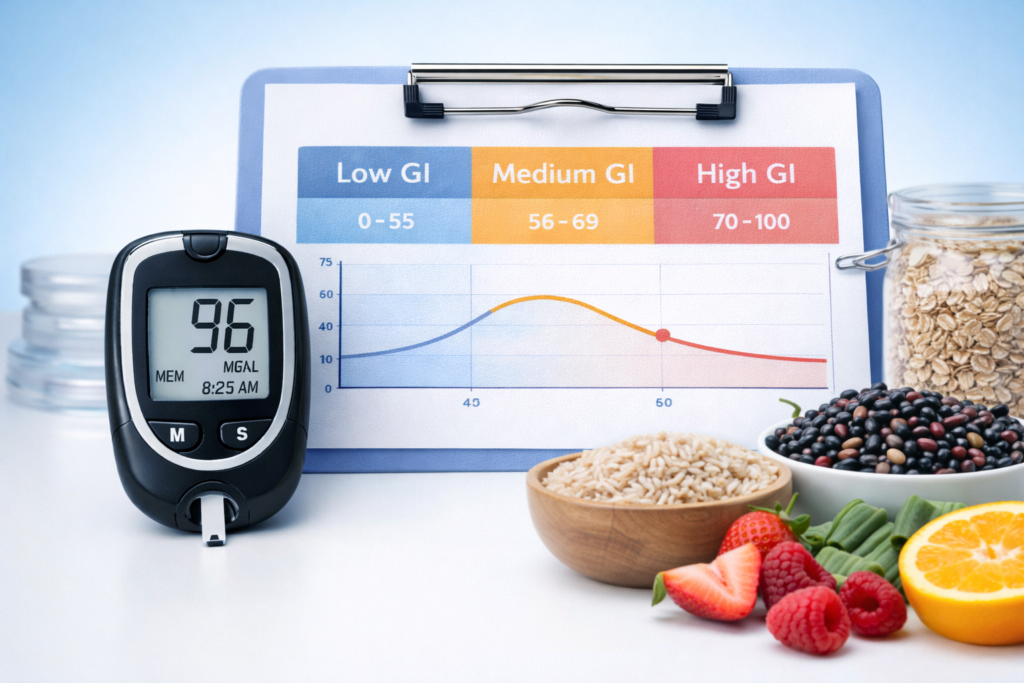
If you are looking for a practical glycemic index guide, the most important thing to know is that the glycemic index, or GI, ranks carbohydrate-containing foods by how quickly they raise blood sugar. That makes it a useful tool inside a broader Blood Sugar Diet strategy, especially for people trying to build meals that lead to steadier glucose levels after eating. Only foods that contain carbohydrate have a GI, and the scale compares how quickly those foods raise blood glucose relative to pure glucose.
But GI is only one part of the picture. It does not tell you how much carbohydrate you are actually eating, and that matters because the amount of carbohydrate in a meal often has a bigger effect on blood sugar than GI alone. That is why this guide works best when paired with practical pages like the Blood Sugar Management Guide and Foods That Help Lower Blood Sugar Naturally, where food quality, portion size, and meal structure all come together.
What Is the Glycemic Index?
The glycemic index is a scale from 0 to 100 that shows how quickly a carbohydrate food tends to raise blood sugar compared with pure glucose, which is assigned a value of 100. In general, lower-GI foods raise glucose more slowly, while higher-GI foods raise it faster.
This matters because not all carbohydrate foods behave the same way in the body. Some are digested and absorbed quickly, which can cause a faster rise in glucose, while others break down more slowly and may lead to a steadier response. That difference becomes especially important for people trying to reduce blood sugar spikes after meals.
Glycemic Index Categories
A practical way to think about GI is in three broad groups:
- Low GI: 0 to 55
- Medium GI: 56 to 69
- High GI: 70 and above
These ranges are useful, but they do not tell you whether a food is automatically healthy or unhealthy. Some lower-GI foods may still be heavily processed or high in calories, while some higher-GI foods may still provide useful nutrients. GI should help guide better choices, not replace overall nutrition judgment.
Low, Medium, and High GI Food Examples
MedlinePlus lists examples that help show the difference:
Lower-GI foods
- barley
- bulgur
- quinoa
- steel-cut or rolled oats
- beans and lentils
- many fruits
- non-starchy vegetables
- milk and yogurt
Medium-GI foods
- couscous
- brown rice
- rye bread
- pita bread
- raisins
- pineapple
Higher-GI foods
- white bread
- bagels
- many processed cereals
- potatoes
- white rice
- sugar
These examples are helpful, but they still need to be used in context. A lower-GI food can still raise blood sugar significantly if the portion is large enough, which is one reason this topic overlaps with Post-Meal Blood Sugar Explained and real-world glucose tracking.
Why the Glycemic Index Can Help Blood Sugar Control
The main benefit of GI is that it can help you choose carbohydrate foods that are less likely to cause a fast, sharp rise in blood sugar. MedlinePlus states that eating more low-GI foods may help people achieve tighter blood sugar control.
This can be especially useful for people who notice repeated blood sugar spikes after refined carbohydrate meals, energy crashes after eating, or a more stable glucose response when meals are built around slower-digesting carbohydrates. GI is not the whole answer, but it can be a smart filter when you are deciding between better and worse carbohydrate choices.
The Biggest Limitation of GI
The biggest mistake people make is assuming that GI is the main thing that determines whether a food is blood sugar friendly.
It is not.
Diabetes UK states clearly that the amount of carbohydrate you eat has a bigger effect on blood sugar than GI alone. That means a large portion of a lower-GI food can still have a greater glucose impact than a small portion of a higher-GI food.
This is one reason GI should not be used in isolation. It works much better when paired with a clearer understanding of post-meal blood sugar and how your body responds to actual meals in daily life. If the portion is too large, the total carbohydrate load can easily overpower the benefit of a lower GI.
Glycemic Index vs. Glycemic Load
A simple way to think about it is this:
- GI tells you how quickly a carbohydrate food tends to raise blood sugar
- Glycemic load gives a better sense of the real blood sugar effect of the portion you actually ate
Diabetes UK explains that glycemic load combines the GI rating with the amount of carbohydrate in the quantity of food. This makes it much more practical in real life, where people eat portions, not laboratory test servings.
If you are still unsure how to interpret these values in practice, it helps to also understand what blood sugar numbers mean across fasting, A1C, and after-meal readings. That bigger framework makes GI much easier to use intelligently.
Why Mixed Meals Change the GI Effect
GI values are usually measured with foods eaten on their own, but real meals are mixed. MedlinePlus notes that combining a higher-GI food with lower-GI foods can change the overall blood sugar effect. Diabetes UK also points out that GI values are based on foods eaten in isolation, even though real meals usually include protein, fat, fiber, and multiple carbohydrate sources.
That means:
- bread with eggs and avocado behaves differently than bread alone
- rice with chicken and vegetables behaves differently than rice alone
- oats with yogurt and nuts behave differently than oats alone
This is one reason whole-meal structure matters more than obsessing over a single GI number.
How to Use GI the Right Way
The best way to use GI is as a supporting food-quality tool, not a rigid rulebook.
1. Prioritize better-quality carbohydrates
ADA recommends choosing carbohydrate foods that are nutrient-dense and rich in fiber, vitamins, and minerals. Whole and minimally processed carbohydrate foods are usually a much better foundation than refined, highly processed carbs.
For more practical food ideas, see Foods That Help Lower Blood Sugar Naturally, which fits naturally with a lower-GI eating pattern.
2. Watch total carbohydrate and portion size
ADA advises paying attention to total carbohydrate on the Nutrition Facts label, and Diabetes UK stresses that carb amount matters more than GI alone.
3. Build mixed meals
ADA’s meal-planning guidance supports building meals with non-starchy vegetables, lean protein, and quality carbohydrate portions rather than letting refined carbs dominate the plate.
4. Monitor your own response
ADA notes that checking how food affects your glucose can help you understand which meals work best for your body. That matters because two people can respond differently to the same food.
5. Use GI for smarter swaps, not food fear
A much better approach is to swap some faster-digesting refined carbs for slower, more fiber-rich options more often, rather than trying to make every meal perfectly “low GI.”
Practical Lower-GI Swaps
A strong real-world strategy is to replace some refined carbohydrate foods with slower-digesting, higher-fiber options where possible.
Examples include:
- steel-cut or rolled oats instead of sugary cereal
- beans or lentils more often instead of refined starchy sides
- more intact grains instead of highly refined snack foods
- fruit, yogurt, nuts, and fiber-rich foods instead of sugary desserts or drinks
If you want to turn these ideas into a more structured routine, the 7-Day Blood Sugar Meal Plan is the logical next step.
Common GI Mistakes to Avoid
Mistake 1: Thinking low GI automatically means healthy
It does not. Some lower-GI foods are still highly processed or less nutritious than they appear.
Mistake 2: Ignoring portion size
This is the biggest one. The total carbohydrate amount usually matters more than GI alone.
Mistake 3: Trusting GI claims on food packaging
ADA says “glycemic index” claims on packages have not been defined by the FDA and should not be relied on as your main decision tool. ADA recommends focusing first on total carbohydrate.
Mistake 4: Forgetting the rest of the meal
Protein, fat, fiber, and the overall meal structure can all change the blood sugar effect. This is why GI should sit inside a broader blood sugar diet strategy rather than becoming the only rule you follow.
Is GI Better Than Carb Counting?
Not really.
GI helps you think about carbohydrate quality, but carb counting or carb awareness helps you think about carbohydrate quantity. MedlinePlus presents GI as a tool to use alongside carb counting, not as a replacement for it. ADA also emphasizes carbohydrate awareness, labels, and meal structure as core parts of blood sugar management.
So for most people:
- GI helps with food quality
- carb awareness helps with quantity
- meal structure helps with consistency
- blood glucose feedback helps with personalization
Who Can Benefit Most From Using GI?
A GI-based strategy can be especially helpful for people who:
- notice larger after-meal rises
- rely heavily on refined carbohydrate foods
- want a more flexible alternative to extreme low-carb eating
- are trying to choose better carbs without overcomplicating meals
- are working on blood sugar spikes and post-meal blood sugar at the same time
This is especially true when reduced carbohydrate tolerance is being driven by deeper metabolic issues such as poor insulin sensitivity. In those cases, food choice matters, but so does the body’s ability to handle glucose efficiently.
The Best Way to Think About GI
The glycemic index is most useful when you use it like this:
- choose more lower-GI, fiber-rich, minimally processed carbohydrate foods
- keep portions sensible
- build balanced mixed meals
- monitor how your own body responds
- do not let GI distract you from the bigger fundamentals of blood sugar control
That is the most practical and sustainable way to apply it.
Conclusion
A strong glycemic index guide should make one thing clear: GI can be helpful for blood sugar control, but it works best when combined with portion awareness, total carbohydrate awareness, meal structure, and real-world glucose feedback. Lower-GI foods can support steadier glucose, but GI alone is not enough to tell you whether a meal is truly blood sugar friendly. Use it as a smart filter, not as the entire system. For readers who want to combine food strategy with symptoms, routines, and long-term glucose stabilization, the Blood Sugar Management Guide brings everything together in one place.
Related Articles
FAQ
1. What is the glycemic index?
The glycemic index, or GI, ranks carbohydrate foods by how quickly they raise blood sugar compared with pure glucose, which is assigned a value of 100.
2. What foods have a GI score?
Only foods that contain carbohydrate have a GI score. Foods like oils, fats, and meats do not have a GI, although they can still affect blood sugar in other ways.
3. What is considered low GI?
Low GI is generally 0 to 55, medium GI is 56 to 69, and high GI is 70 and above.
4. Does low GI always mean healthy?
No. Diabetes UK notes that not all low-GI foods are healthy choices, and not all high-GI foods are unhealthy choices.
5. Is the glycemic index more important than portion size?
No. Diabetes UK says the amount of carbohydrate you eat has a bigger effect on blood sugar than GI alone.
6. What is glycemic load?
Glycemic load combines the GI of a food with the amount of carbohydrate in the portion you actually eat.
7. Can mixed meals change the GI effect?
Yes. MedlinePlus says the impact of a food can change when it is combined with other foods, and Diabetes UK notes that GI values are based on foods eaten on their own rather than as mixed meals.
8. Should I trust “glycemic index” claims on food packages?
ADA says GI claims on food packages have not been defined by the FDA and the ADA does not recommend relying on them. It recommends checking total carbohydrate first.
9. Is GI better than carb counting?
Not really. GI can help with carbohydrate quality, but MedlinePlus and ADA both support using it alongside carbohydrate awareness, not as a replacement.
10. What is the easiest way to use GI in real life?
Choose more lower-GI, higher-fiber, minimally processed carbohydrate foods, keep portions sensible, and build mixed meals using a structure like the Diabetes Plate.
Use the Glycemic Index More Effectively
GI is useful, but it works best when you combine it with better meal structure, portion awareness, and blood sugar feedback. Start with the main diet pillar, then go deeper into food choices and daily control.
Written by Blood Sugar Insider Editorial Team
Health researchers and writers specializing in blood sugar control, metabolic health, and evidence-based nutrition.
Our editorial team creates evidence-based content designed to help readers understand blood sugar balance, prevent spikes, and support long-term metabolic health using science-backed strategies.
Medically Reviewed for Accuracy
This content has been reviewed for accuracy and clarity by the Blood Sugar Insider Medical Review Team, using current clinical research and evidence-based guidelines.
Our process ensures that information related to blood sugar, metabolism, and health strategies aligns with current scientific understanding and evidence-based practices.
View our Editorial Policy →