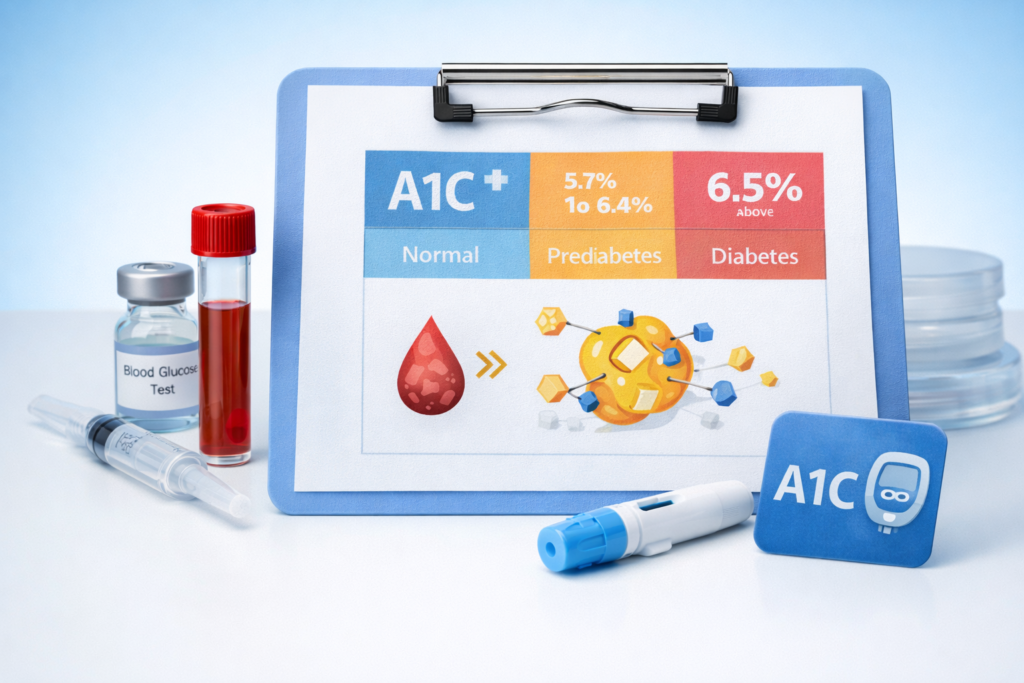
If you need A1C explained in simple terms, A1C is a blood test that reflects your average blood sugar over time rather than what your glucose is doing at one single moment. It is one of the most important tools in the Blood Sugar Basics section because it helps show the longer pattern behind your blood sugar, not just a one-time reading.
That is also why A1C should never be viewed as the only number that matters. A1C does not show how high your blood sugar rises after a specific meal or whether fasting glucose is drifting upward, which is why it makes the most sense when compared with Fasting Blood Sugar Explained and What Blood Sugar Numbers Mean.
What Is A1C?
A1C is also called hemoglobin A1C, HbA1C, glycated hemoglobin, or glycosylated hemoglobin. When glucose enters the bloodstream, some of it attaches to hemoglobin inside red blood cells. The A1C test measures the percentage of hemoglobin that is “sugar-coated,” which is why higher long-term glucose exposure produces a higher A1C percentage.
Because red blood cells turn over over time, A1C works like a rolling average rather than a real-time reading. That makes it useful for spotting long-term trends, but less useful for understanding what happened after one specific meal, bad night of sleep, or stressful day.
What Is a Normal A1C?
For most nonpregnant adults, the standard diagnostic A1C ranges are:
Normal: below 5.7%
Prediabetes: 5.7% to 6.4%
Diabetes: 6.5% or above
That means:
- an A1C of 5.4% is usually considered normal
- an A1C of 5.9% is in the prediabetes range
- an A1C of 6.7% is in the diabetes range, pending proper clinical confirmation where needed
A1C Range Chart
A1C Result | What It Usually Means
- Below 5.7%: Normal
- 5.7% to 6.4%: Prediabetes
- 6.5% or above: Diabetes range
These are the standard CDC and NIDDK diagnostic cutoffs used for most nonpregnant adults.
What Does A1C Actually Tell You?
A1C tells you whether your blood sugar has been running higher than normal over time. It is not the same as checking your glucose once with a fingerstick or lab fasting test. A fasting glucose test tells you what your blood sugar is at one point in time, while A1C shows the average pattern over the previous few months.
That is why A1C can sometimes reveal an issue even when a single fasting test looks acceptable. The reverse can also happen: NIDDK notes that in some people, a blood glucose test can indicate diabetes even though an A1C test does not, and vice versa.
A1C vs. Fasting Blood Sugar
These two tests work together, but they are not interchangeable.
- A1C reflects average glucose over roughly 3 months
- Fasting blood sugar measures glucose at the moment of the blood draw after fasting
- A1C does not require fasting
- Fasting glucose is more immediate, while A1C is more long-range
NIDDK’s professional guidance notes that fasting plasma glucose can be more sensitive than A1C for some people, while the oral glucose tolerance test is even more sensitive. That is one reason why a normal or borderline A1C does not always rule out other blood sugar problems.
If you want the side-by-side version, pair this page with:
- Fasting Blood Sugar Explained
- What Blood Sugar Numbers Mean
- What Are Normal Blood Sugar Levels by Age?
A1C and Estimated Average Glucose (eAG)
ADA explains that A1C can also be reported as estimated average glucose, or eAG, which converts the percentage into the same mg/dL-style units many people see on glucose meters. For example, ADA notes that an A1C of 7% corresponds to an estimated average glucose of about 154 mg/dL.
This can make A1C easier to understand, but it still remains an average. An average can hide wide swings. Someone could have a middling A1C while still having large post-meal spikes and crashes. That is one reason CGM or paired glucose testing can add useful context. ADA’s time-in-range guidance also emphasizes that pattern quality matters, not just averages.
Why A1C Matters
A1C matters because it helps identify prediabetes and diabetes, and it is also widely used to monitor long-term glucose control in people who already have diabetes. CDC describes prediabetes as a serious health condition that increases the risk of type 2 diabetes, heart disease, and stroke, so an A1C in the prediabetes range should not be brushed off as trivial.
A rising A1C can also be an early signal that insulin resistance is building in the background. NIDDK’s guidance on insulin resistance and prediabetes explicitly links A1C testing to that broader metabolic picture.
When A1C Can Be Misleading
A1C is useful, but there are situations where it may not reflect your true glucose status accurately.
CDC says A1C accuracy can be affected by:
- severe anemia
- kidney failure
- liver disease
- certain blood disorders such as sickle cell anemia or thalassemia
- certain medicines, including some opioids and HIV medications
- blood loss or blood transfusions
- early or late pregnancy
NIDDK also notes that certain hemoglobin variants can interfere with some A1C methods, and that if your A1C result does not match your blood glucose levels, clinicians should consider whether A1C is reliable for you. Most commonly used tests in the United States are not affected by the most common variants, but this still matters in some patients.
NIDDK further notes that A1C can be falsely high in people who are very low in iron, such as those with iron-deficiency anemia, and can also be affected by kidney failure or liver disease.
What Is a Good A1C If You Already Have Diabetes?
For many nonpregnant adults living with diabetes, ADA generally suggests an A1C goal of 7%. ADA also stresses that goals are individualized, and more or less stringent targets may be appropriate depending on age, overall health, risk of hypoglycemia, and other clinical factors.
That target is different from what counts as normal in someone who has not been diagnosed. This distinction matters:
- Normal / diagnostic A1C: below 5.7%
- Common diabetes management target: around 7% for many adults, individualized by context
Can You Have a Normal A1C and Still Have Blood Sugar Problems?
Yes.
NIDDK notes that blood glucose tests and A1C do not always agree. Some people may have a blood glucose test suggesting diabetes even though A1C does not, and the reverse can also happen. NIDDK also notes that A1C may miss prediabetes in some people with certain health conditions.
This is why a “normal” A1C should not automatically end the conversation if:
- fasting glucose is high
- post-meal spikes are obvious
- symptoms are present
- CGM data looks abnormal
- insulin resistance signs are building
What To Do If Your A1C Is High
If your A1C is elevated, the first step is not panic. It is interpretation and action.
NIDDK says healthy living may help prevent or reverse insulin resistance and prediabetes, including healthy food and drink choices, physical activity, weight management, and enough sleep. NIH-funded Diabetes Prevention Program findings also showed that losing 5% to 7% of starting body weight lowered type 2 diabetes risk in high-risk adults.
That makes these next steps practical:
- improve sleep quality
- reduce refined carbohydrate overload
- walk after meals
- improve insulin sensitivity through movement and resistance training
- compare A1C with fasting and post-meal data
- look for root causes instead of focusing on a single number
Good next pages:
- Blood Sugar Basics
- Fasting Blood Sugar Explained
- Post-Meal Blood Sugar Explained
- What Is Insulin Resistance
- Blood Sugar Management Guide
When To Speak With a Doctor
You should follow up with a healthcare professional when:
- your A1C is 5.7% or higher
- your result does not match your fasting glucose or symptoms
- you have risk factors for diabetes or prediabetes
- you have anemia, kidney disease, liver disease, a hemoglobin disorder, or another condition that could affect A1C accuracy
- you are pregnant or recently had major blood loss or transfusion
Conclusion
If you needed A1C explained, the simplest summary is this: A1C is a blood test that estimates your average blood sugar over the past few months, it does not require fasting, and the key diagnostic ranges are below 5.7% for normal, 5.7% to 6.4% for prediabetes, and 6.5% or above for diabetes. It is one of the most useful long-range blood sugar tests, but it works best when interpreted alongside fasting glucose, symptoms, and the broader picture of insulin resistance and daily glucose patterns.
Related Articles
FAQ
What does A1C measure?
A1C measures the percentage of hemoglobin in your red blood cells that has glucose attached to it, which reflects your average blood sugar over the past 2 to 3 months.
What is a normal A1C?
For most nonpregnant adults, a normal A1C is below 5.7%.
What A1C level means prediabetes?
An A1C of 5.7% to 6.4% is in the prediabetes range.
What A1C level means diabetes?
An A1C of 6.5% or above is in the diabetes range.
Do you need to fast for an A1C test?
No. You do not need to fast before an A1C blood test.
Is A1C the same as a fasting blood sugar test?
No. A1C reflects average blood sugar over a few months, while fasting glucose is a one-time reading after an overnight fast.
Can A1C be wrong or misleading?
Yes. A1C can be less accurate in some people, including those with severe anemia, kidney failure, liver disease, blood loss, transfusions, pregnancy-related changes, or some hemoglobin variants.
What is eAG?
eAG stands for estimated average glucose. ADA explains that it converts an A1C percentage into a blood-glucose-style average, such as mg/dL.
Is an A1C of 6.0 bad?
An A1C of 6.0% falls in the prediabetes range, not the normal range.
What A1C target is common for adults with diabetes?
ADA generally suggests an A1C goal of 7% for many nonpregnant adults with diabetes, while emphasizing that goals should be individualized.
See What Your A1C Means in the Bigger Picture
A1C is powerful, but it is only one part of the story. Compare it with fasting glucose, symptoms, and the deeper drivers behind blood sugar imbalance.
Written by Blood Sugar Insider Editorial Team
Health researchers and writers specializing in blood sugar control, metabolic health, and evidence-based nutrition.
Our editorial team creates evidence-based content designed to help readers understand blood sugar balance, prevent spikes, and support long-term metabolic health using science-backed strategies.
Medically Reviewed for Accuracy
This content has been reviewed for accuracy and clarity by the Blood Sugar Insider Medical Review Team, using current clinical research and evidence-based guidelines.
Our process ensures that information related to blood sugar, metabolism, and health strategies aligns with current scientific understanding and evidence-based practices.
View our Editorial Policy →